Personal Agency is Key to Individual Wellbeing and to Organisational Change
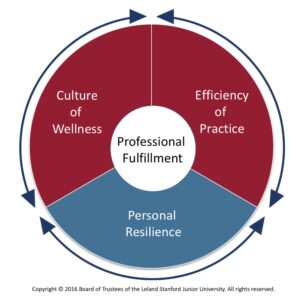
According to the Stanford WellMD model of healthcare, healthcare worker well being1 is achieved from 20% personal resilience and 80% organisational responsibility (changing systems and structures in the workplace).
The Stanford research is impressive and guides a great deal of our work. It’s impact in helping healthcare organisations to get serious about their responsibilities to their people, is huge and vital. (We all accept that burnout is caused by poor workplace management.)
The Stanford model says “while the organization is responsible for the majority of factors related to well-being, the individual still plays a critical role. Personal Resilience refers to the individual skills, behaviors, and attitudes that contribute to physical, emotional, and professional well-being”. 2
I have just one concern with these percentages. It’s not with the research, I am grateful someone is seeking to measure what is really happening to healthcare workers, to understand what our systems are doing to our people. Mostly because organisations, Boards and Leaders, will only attend to what they can measure.
My concern is that many doctors ignore the above sentence about individuals playing a ‘critical role’ in wellbeing, leading to two problems.
The first is, that many people see that 20% figure and lose their individual motivation to do something about their own wellbeing. When that happens, when we withdraw our own personal agency, the second problem arises. We don’t build the skills we need to impact change, making us ineffective in the short and long term. Potentially leading to helplessness, disappointment, disengagement and resentment.
It is a challenging paradox, perhaps a chicken and egg problem. Do we need the systems to change first so we feel valued and can then do our best work, or do we need to build our own capacity first, so we can argue for the systems change and be part of creating it.
Of course, we need both. For doctors to have a seat at the table, to have a voice, they need certain skills. Skills in:
- describing the problem and the aspired future
- emotional intelligence
- collaboration and partnership
- personal well being, an ability to meet one’s own psychological needs
Adults have three basic psychological needs – autonomy, competence and relatedness. We want to feel like we belong, which is part of feeling safe, that we are the drivers of our own lives, and that we are able to achieve whatever is important to us. I fear for those who abdicate their foundational psychological needs to the system or some mysterious group of unknown, so called systems leaders. Neither the system nor those in leadership roles can truly see you as an individual. That is your job. The 20% you are responsible for is foundational and essential to your wellbeing and to your organisation’s. The experience of one’s own agency, of believing that I can do something to improve my lot, is powerful and can be energising, generating creativity and hope for ourselves and for the collective.
Perhaps the collective state of healthcare workers now at the end of the fourth year of a pandemic, is simply too exhausted to do anything more than point to the system.
Individual responsibility is a tough message to hear, especially if you are exhausted. It seems easier to say it’s the system and to hope, now that we all agree there is a problem, that someone will fix it.
The problem is that when you say ‘it’s the system’, as if that is the whole story, you abdicate your wellbeing to an entity that has no interest or care in you as an individual. For you to have the life you want, you need to be actively engaged in it. No one else cares as much about your life as you do, except perhaps your mum or dad….
Worker well being is the essential ingredient for healthcare organisations to meet every one of their KPIs and has largely been ignored. Many of us have been saying this for years. Wellbeing and performance are NOT separate and never have been. Workforce pressures and post COVID attitude changes, have now made the phrase employer of choice, a reality that cannot be so easily ignored by healthcare employers.
I am lucky to know some doctors who work in amazing teams that are psychologically safe and where people want to come to work. Success begets success, because the positions are filled and people are fulfilled in their work, they don’t leave. Over time the team becomes more effective, more reliable, and the work continues to be meaningful, because it exists on a foundation of connection. People feel valued and look out for each other. They are creating a virtuous cycle, an effective system, in their unit.
Will the system interrupt itself and create something different? No. That will only happen when a small group of people with individual skill, capacity and voice activate and decide to interrupt it. And it turns out, lots of small ways at the unit level, will likely trump a big organisation wide program of change.3
Can the organisation help or hinder this team’s efforts? Of course, both-and is the required lens to use. And, the leadership must enable the unit team if they want to keep a workforce that will allow the organisation to continue to exist.
Burnt out or unwell workers impede efforts to improve healthcare, they are a safety and quality risk to patients and the organisation. If a healthcare worker is not able to behave as a human being who needs a rest occasionally, who needs to be with their loved ones when they feel vulnerable, feel valued for their contribution in difficult circumstances, then they are likely to become resentful, cynical and to reduce their discretionary effort. It is morally and financially unsustainable for the organisation to do nothing. Worker wellbeing is no longer an optional extra.
Recently I had the privilege of speaking to a room of people about the individual skills one can develop to enhance their wellbeing. The other four presentations focused on culture, structure and systems for wellbeing. In light of the Stanford research, you might say the speaker ratio was about right at 80% – 20%. If our organisations can deliver what the others talked about, our healthcare system will be unrecognisably better in every way.
For now, the system is producing exactly the results it is designed to deliver, it is no longer fit for purpose. We need a BOTH – AND approach. For the system to change, collections of individuals will need to raise their skills, muster their determined will and dig deep. Many of us are tired, no one can address the system on their own.
Don’t wait for the system, build your skills so that you can be the system. So that you can build the system you want to work in. If you are a leader get serious immediately about being the employer of choice, before you find out it’s too late. Coaching is one way to raise your accountability, capacity, clarity and focus. Fostering a coaching culture widely in your organisation will amplify the impact.
Ron Barassi, Australian Football League legend, player and coach lived by the creed:
“If it is to be, it is up to me”.
Ron Barassi
Barassi won 10 Aussie Rules premierships as player and coach. He was known for never running away, and for his kindness and humour. He was given a State funeral this week as a well loved, role model, well beyond football circles.
Ron worked for decades in teams as a leader and took responsibility for the ups and downs of his life. His belief in himself and his responsibility for himself, did not excuse the team or the organisation. It’s my proposal that it kept him engaged.
Ron worked with four clubs over his career, nothing was static, it was not all plain sailing. By all accounts it was a life well lived, closely connected to others and on his terms. Ron was activated, he didn’t wait for someone else to deliver, he understood he could impact the world around him and that he needed to work with others.
Are you willing to build the skills you need to create the life you really want? A life of connection, autonomy and achievement. One that also helps others create their version of the life they really want. What would happen to our collective, our organisations if we did?
Start with your own wellbeing skills, what’s one thing you can do today to take better care or yourself, to value your life, time and effort?
Footnote:
Healthcare worker well being is referred to as professional fulfillment at Standford
https://wellmd.stanford.edu/about/model-external.html
https://www.mayoclinicproceedings.org/article/S0025-6196(22)00650-4/fulltext
References
https://wellmd.stanford.edu/about/model-external.html

The Thriving Doctor
Sharee Johnson’s book The Thriving Doctor is available in all good bookstores or online.
Sharee has been coaching doctors since 2014, find out more about her work